Back pain & neck pain
Herniated disc (neck or back)
A herniated disc is one of the most common spine disorders. We make a distinction between herniated discs in the back (= lumbar herniated disc) and in the neck (= cervical herniated disc).
What is a herniated disc?
Before elaborating on the treatment of this condition, it may be wise to reflect on what exactly a herniated or slipped disc is.
In between our vertebrae, we have a discus-shaped disc that ensures that the vertebrae do not make contact with one another and facilitates mutual movements. This intervertebral disc consists of an outer ring of solid, fibrous cartilage and a weak, jelly-like nucleus. It is this nucleus that creates the elasticity and shock-absorbing effect of the spine during movements.
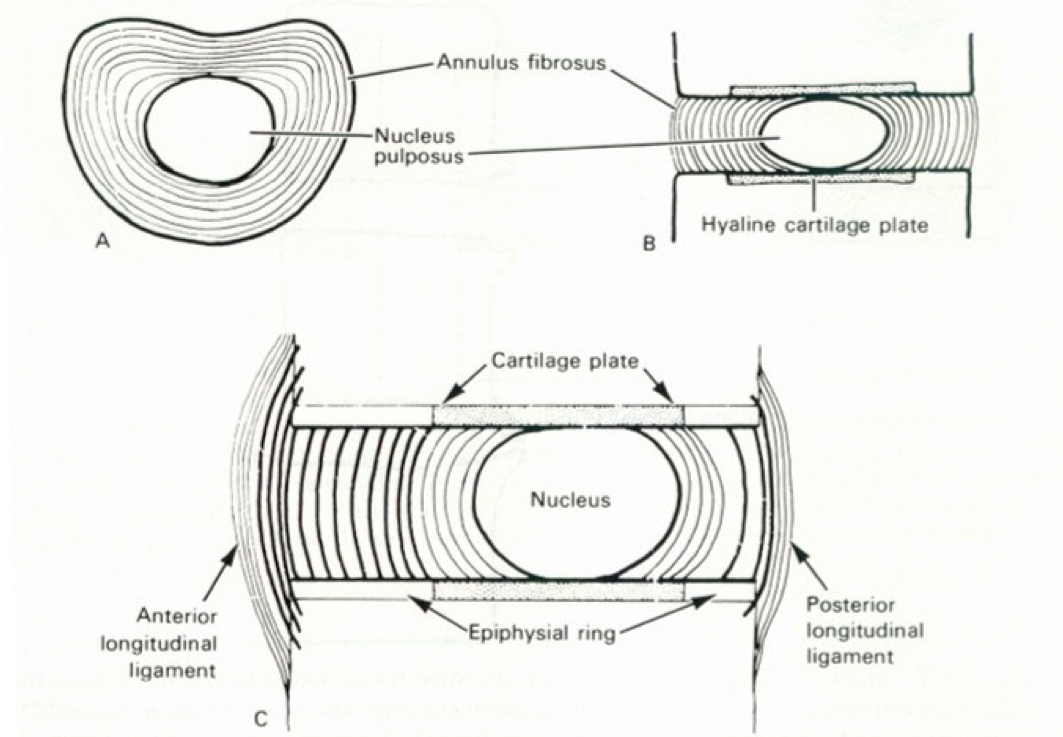
When the outer ring (annulus) of the intervertebral disc ruptures (e.g. following too much strain on the back, a wrong movement or an accident), the jelly-like nucleus may bulge and thus irritate or even partly pinch the nerve. This results in radiating pain in legs or arms. In a worst-case scenario, it may even lead to signs of paralysis.
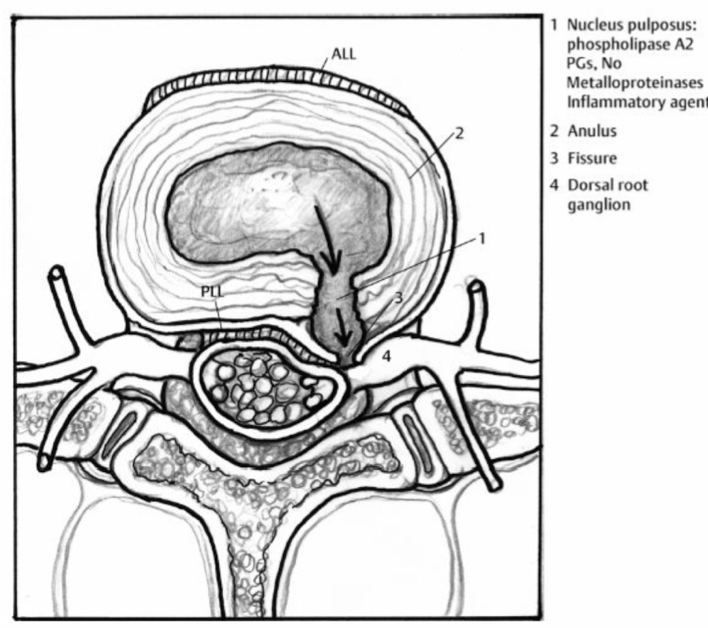
The name ‘herniated disc' comes from Latin and means ‘fracture'; this term refers to the protrusion or rupturing of the annulus of the intervertebral disc.
Lumbar and cervical herniated disc
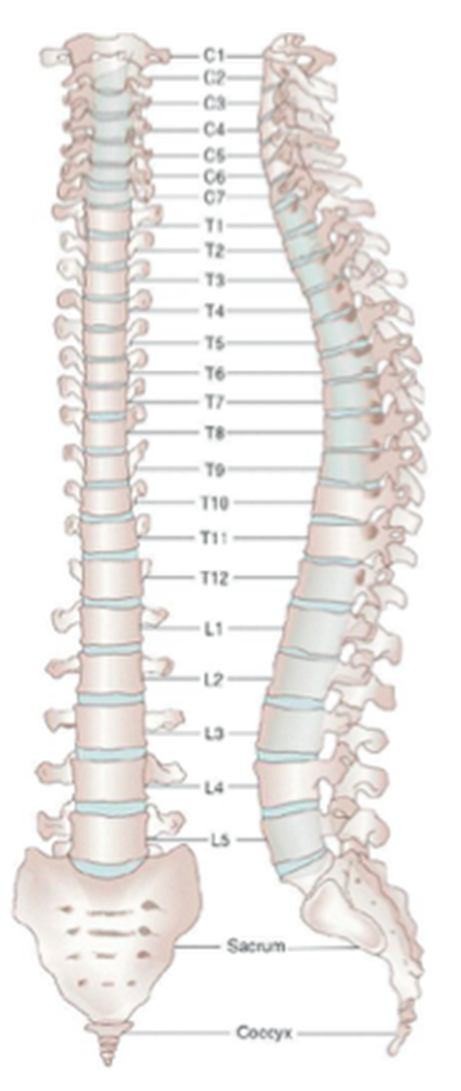
Most herniated discs occur in the lower three segments of the spine (= lumbar herniated disc) but cervical herniated
discs are not uncommon either.
The protrusion of the intervertebral disc may press directly on a nerve root and thus cause intense pain. Furthermore,
a nerve that is being pinched for too long might become permanently damaged, resulting in chronic pain, sensation
disorders and paralysis. Because of this, it is often recommended to surgically remove the protrusion so that the
nerve function is restored and the patient's complaints diminish or disappear.
Minimally invasive technique for less pain and faster recovery
In the OLV Hospital, we standardly use a ‘discectomy by way of transmuscular tubes' (very small tubes) for back surgery, using a surgical microscope or an endoscope (micro-endoscopic discectomy or MED).
This 'keyhole surgery' or ‘minimally invasive technique' ensures that the tissue is affected as little as possible. Patients will suffer less pain, can leave the hospital earlier and will recover sooner.
Back surgery in the past: invasive and painful
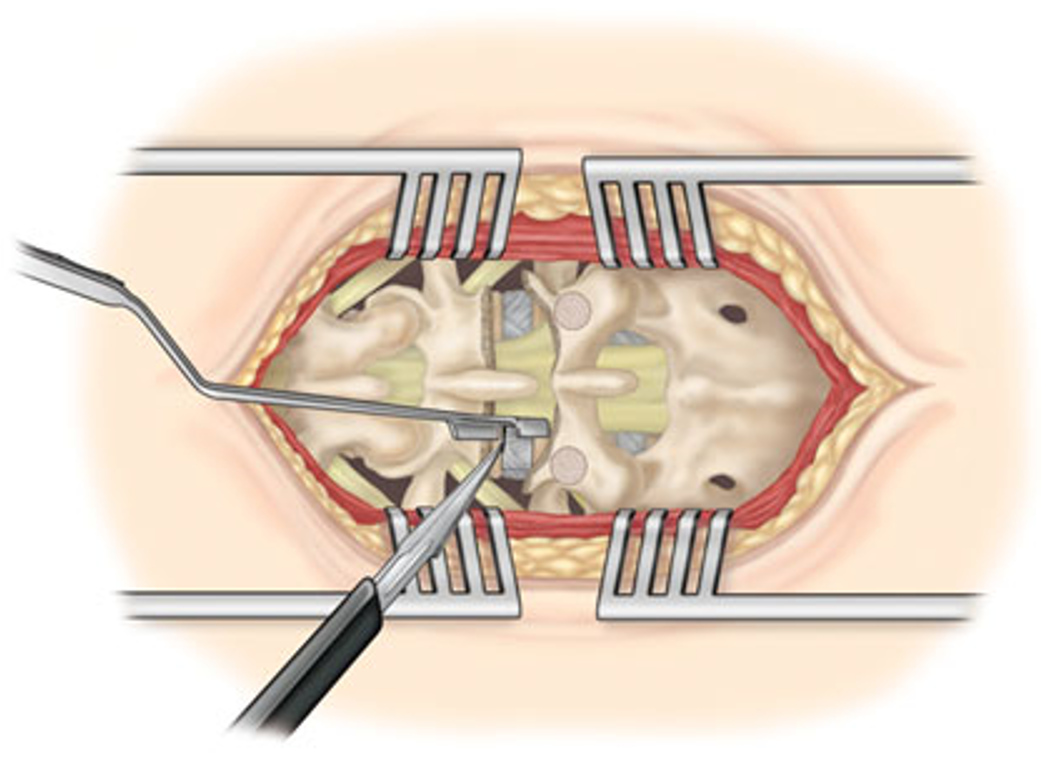
Above: the traditional incision: the muscles had to be spread far apart, which led to major pain complaints after surgery.
Back surgery today: minimally invasive for faster recovery
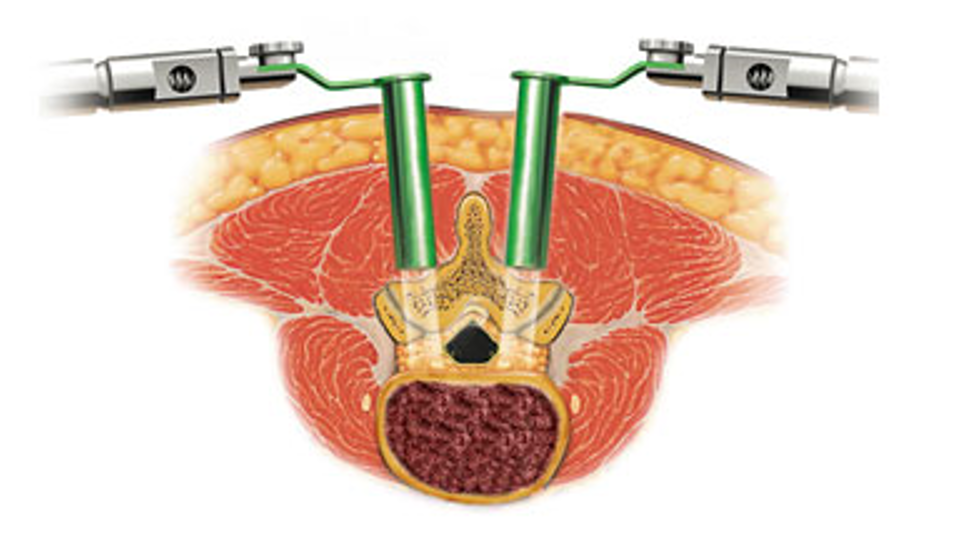
Surgery for herniated disc in the back (lumbar herniated disc)
If pain treatment and rest cannot relieve the complaints, surgery is often the last resort. Whereas a herniated disc operation used to be an invasive medical intervention, this is today fortunately a completely different story. Herniated discs are surgically removed using a transmuscular tube and a microscope or endoscope. This procedure is called micro-endoscopic discectomy (MED).
In this procedure, mini-tubes are led into the back, through a very small incision in the skin at the herniated intervertebral disc.
The protrusion of the disc is removed through these tubes using fine instruments. This will immediately decrease the pressure on the nerve, as a result of which also the pain will immediately diminish or even disappear completely.
Video
Brochure
Here, you can consult our brochure with recommendations after lumbar herniated disc surgery.
Removing a herniated disc in the neck (cervical herniated disc)
A cervical herniated disc is quite similar to a lumbar herniated disc: it is a protrusion of the softer inner core of the intervertebral disc causing pressure on the nerve and radiating pain in the arm. The presence of spinal cord at the cervical vertebrae constitutes an additional risk. If the herniated disc presses against the spinal cord, surgery is inevitable. If the herniated disc solely exercises pressure on the nerve, the same rules as for a lumbar herniated disc apply: surgery will be suggested if the pain does not disappear after a pain treatment period.
The surgical procedure differs from that in the lower back. For most patients, the operation will be executed along the front side of the spinal column (i.e. through the throat). Usually, the intervertebral disc is almost completely removed. Because the herniated disc (= intervertebral disc) is fully removed, it will in most cases be replaced by a prosthesis. These so-called cages are made from biologically compatible material and filled with artificial bone or bone from the bone bank.
Meanwhile, much progress has been made in the development of biologically compatible materials. These are materials that do not cause a reaction in the human body.

|
Here, the cage is made from PEEK (based on carbon fibres) but also titanium is commonly used.
|
In some cases, for instance when several disc levels must be operated, it may be necessary to insert an additional reinforcement in between several vertebrae. This is done by securing a small metal plate with screws on the front side of the vertebrae. Your surgeon will discuss the necessity of this procedure with you prior to the operation.
However, reinforcing a segment also has disadvantages. The intervertebral discs above and below the reinforced segment may become subject to wear sooner, which may cause a new herniated disc. But this is definitely not always the case.
Usually, the results of this surgical procedure are excellent, hospitalisation is short (as a standard, 1 overnight stay after the operation).
Video
Brochure
Here, you can consult our brochure with recommendations after cervical herniated disc surgery.
